Markerless Motion Capture 101
- Oct 12, 2018
- 5 min read
Updated: Apr 3, 2019
In this post we'll examine markerless motion capture in the context of the PT clinic.
First things first.
What is motion capture?
Motion capture (mocap) refers to the process of recording, and quantifying motion. We will discuss motion capture In the context of physical therapy in this post - i.e. human motion analysis.
Typically mocap involves at least one color camera or one or more wearable sensors. Color cameras, depth sensing cameras, wearables in accelerometers, gyroscopes, reflective markers, or electromagnetic markers can be combined to form a computerized construction of the human skeleton in 3D. The raw data gathered from hardware is then processed by motion analysis software.
Motion capture technology was initially adopted by Hollywood studios, and university biomechanics labs. Intense, highly-specialized labor was required to extract meaningful information out of these traditional systems.
Now with the spread of ever more powerful hardware, and software, motion capture and analysis technology has become accessible for the PT clinic.
Why does motion capture make sense for a PT clinic?
There are both health outcomes, and business results benefits.
A motion capture system can be used to champion excellence of care and evidence based-practice for your physical therapy clinic. Using an objective method of tracking and quantifying patient movement enables the longitudinal tracking of patient progress. Now that the clinic has a systematic way of tracking progress, the clinician can decide for themselves whether the course of treatment in and outside the clinic is getting their patients better. Providing the health professional with the right information has been shown to improve health outcomes [1].
From the business perspective, a motion capture tool can be used to provide new services to cater to current, or perhaps new groups of customers. For example, mocap enabled movement screens could be used to build in-roads with the local athletic teams.
Empowering the clinician with a tool that can be used to educate the patient patient, better engage them, and better retain them as a customer is a strong reason to consider this product for your clinic.
Finally, physical therapy clinics looking to differentiate themselves in front of referring physicians can use motion analysis to demonstrate that they are the forefront of physical therapy operations. Unlike a piece of hardware, if applied in the right way, motion analysis is concrete evidence that the clinic is at the forefront of applying technology to further the patient experience and patient health outcomes.
Unlike specialized pieces of hardware, a motion analysis system can be integrated into the operations flow for a large segment of patients. Orthopaedic, geriatric, and sports patients are examples of patient groups, where motion analysis can help clinician and patient.
What is the best motion capture system for a PT clinic?
It depends!
If you are looking for a biomechanics-lab grade (the gold standard in measurement) system with the highest possible accuracy and frame-rate capture, look at traditional motion capture systems. These types of systems are distinguished by multiple cameras, and multiple markers, and a heavy need for real estate. Recording sprints, fast and dynamic cutting motions, and baseball pitches are all possible, albeit at a cost of complex and operationally intensive setup, operations, and post-processing time.
If you are looking for a system more suitable for outdoors recording, consider inertial measurement units (IMUs), or electromagnetic measurements units (EMUs). The wearable nature of these devices makes them portable. They can be good for high speed motion - e.g. a baseball pitch. They do require some degree of setup, and post-operational processing in downloading data, and accounting for setup and operational accuracy errors.
If you are looking for a system for your clinic, you could consider the two above options, and also a markerless motion capture system. Markerless systems defining feature is that there is no need for wearable sensors or markers. Generally this decreases both setup and operations time. Markerless mocap systems can consist of multiple cameras, or a single sensor (i.e. a combined color + depth sensor - we use this setup at EuMotus). Below is a video of a sample movement screen using our system.
2D video motion analysis (e.g. a cell phone) can be used to record qualitative evidence of movement faults (e.g. major knee valgus), and is low-cost, portable, and easily transferable to the field. Due to the nature of 2D camera perception, this method cannot be used to systematically and objectively quantify AROM across multiple body joints.
To learn more about the various types of systems, consider taking our 3D markerless motion analysis CEU course.
Download Your Free Markerless Motion Capture 101 E-book Below!
What are the trade-offs of a markerless motion capture system?
While these systems are not as accurate as gold standard mocap systems, they score well and are reliable, valid. Markerless mocap is more accurate than unaided visual observation, or manual single joint PROM measurement (i.e. goniometry).
The key enabler for a markerless mocap system in the clinical context is speed of setup, speed of operations, and minimization/elimination of post-processing. Clinicians have limited, precious time with their customers. If the time it takes to set up, run, and post-process a mocap system run is greater than the patient’s appointment duration, then this system would not fit into the operational flow of a clinic. This ‘high fidelity’ scenario is plausible where a client pays for an extended specialized motion capture session / package of sessions. The ‘high fidelity scenario’, does not fit in the average PT clinic operation, but could fit in your context.
The EuMotus markerless motion capture system consists of simply one 3D sensor - a combined color camera and depth sensor. A general rule-of-thumb is that the less sensors, and wearables, the simpler and quicker the operation.
Here is a set of questions you can use to evaluate various types of motion capture systems.
So what does markerless motion capture in the clinical setting look like?
In this example, we'll walk you through how a EuMotus customer might use our mocap system in their clinic.
The patient steps through the door and checks in. The PT then selects a set of exercises that are personalized to the patient. For example, for a post-op ACL patient, the clinician selects overhead squat, or even a single hop test. For a geriatrics patient, the clinician could choose a combination of lower and upper extremity AROM tests, and a balance test.
Immediately after the exercises are performed, active range of motion, functional (a)symmetry, and movement stability (e.g. presence of knee valgus during squat etc.) results are displayed.
The clinician also has a video review tool at their disposal to engage and educate their patient, by teaching them through video playback. Designed for the clinician, EuMotus software also allows side-by-side plotting of movement metrics of interest (e.g. elbow flexion, pelvic rotation etc.)
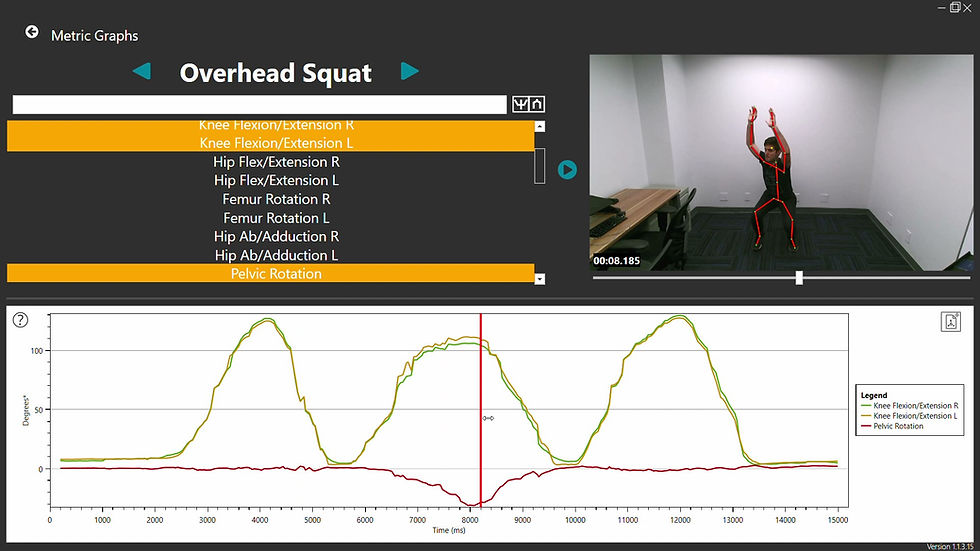
Doesn’t it take too long to run in a clinical setting?
It depends on the setup!
IMUs may take a while to set up. A multi-camera system could take an even longer amount of time to setup, and post-process. With EuMotus markerless motion capture, clients run movement screens in as little as 1-2 minutes, which makes it practical for most PT clinics.
Are markerless motion capture systems portable?
Yes! The EuMotus system is portable, and can be taken down and set up in a few minutes.
Are markerless mocap systems accurate, repeatable, and valid?
Yes! For evidence on single 3D sensor markerless motion capture, read on at our evidence page.
Have more questions?
Check out our FAQ page, or contact us at hello/at/eumotus/com.
Download Your Free Markerless Motion Capture 101 E-book Below!
References
[1] Finkelstein J, Knight A, Marinopoulos S, Gibbons MC, Berger Z, Aboumatar H, Wilson RF, Lau BD, Sharma R, Bass EB. Enabling patient-centered care through health information technology. Evid Rep Technol Assess (Full Rep). 2012 Jun;(206):1-1531.
.png)



The application feels very organized because important gaming features are easy to locate without unnecessary searching or confusion. Navigation remains smooth throughout the platform, helping users enjoy the experience more comfortably on Android devices. I appreciate how visually balanced the interface feels during regular usage. The overall layout creates a practical and engaging mobile environment.
Raja Game download
This article provides important insights into the enhancement of academic writing.
Utilizing strategies such as reading aloud, obtaining feedback, and prioritizing clarity can greatly enhance writing abilities.
Moreover, investigating resources on how to improve your academic writing skills can offer organized guidance and further elevate one's writing proficiency.
Discover the ideal companion for your evening or special occasion with a charming Escort in AIIMS. She brings elegance, intelligence, and a delightful presence to every encounter. Her commitment to your satisfaction ensures a comfortable and engaging atmosphere, making your time spent together truly unforgettable and perfectly tailored to your needs.
Cinsel Sohbet Ve Cinael Chat Uygulaması.
Toplumun her kesimine hitap ederek bireylerin huzurlu, güvenli ve mutlu paylaşımlarda bulunmasını sağlamak, kişiler arası iletişimi, sosyal ve kültürel paylaşımı arttırarak toplumun psikososyal durumunu iyileştirmek, samimi, gerçek ve duygu yoğunluğu olan arkadaşlıkları teşvik ederek, kişiler arası yardımlaşmanın önemini kavratmak, hayatın her anını tüm güzellikleriyle kullancıların eş zamanlı birlikte yaşamasını sağlamak.https://www.gevezeyeri.com/cinselsohbet.html
Sosyal paylaşım ve Cinsel sohbet Odalarımızı ziyaret eden her kullanıcının farklı alanlardaki ihtiyaçlarına cevap verebilmek, günlük hayatın problemlerinden ve iş stresinden uzaklaşabilecekleri hobi alanları yaratmak, dünyadan ve ulusal gelişmelerden aktüel haberleri kullanıcıların takip etmesini sağlayarak toplumun bilinçlenmesine katkıda bulunmak, sevgi, saygı, huzur ve hoşgörü temeline dayanan gerçekçi bir cinsel sohbet platformu olmak.https://www.gevezeyeri.com/gabilesohbet.html
Keyifli ve eğlenceli dakikalar gecireceginiz Gabile Chat odaları günün her saati ücretsiz olarak…